Many problems of the spine are resulting from degeneration of the intervertebral disc. Different postures and movements can cause changing pressure on the intervertebral disc. Especially movements with a bold back have a bulging effect on the intervertebral disc to the back. In the figure we see that the pressure on the intervertebral disc can vary from 25 to 275 kg depending on different postures. If back pain is caused by an irritated intervertebral disc, it can clearly be stated that lying down will relief the pain and constantly sitting in a low soft chair (think of the car seat) will cause most complaints. Forward bending postures (think of working at a low kitchen unit) will cause a high pressure on the intervertebral disc which is directed backwards.
On the photo: intradiscal pressure on the third lumbar intervertebral disc in the following postures (left to right): supine position, lateral position, standing, standing 20 degrees bent over, same with a weight of 20 kg, sitting without support, sitting 20 degrees bent over and the same with a weight of 20 kg. (according to Nachemson)
The nightmare, the often discussed Hernia
The following story shows how the changes in the intervertebral disc can lead to a hernia. It is obvious that this is a final stage and the complaints belong to specific back pains. After a simple examination your physiotherapist can easily tell you if he is thinking of a hernia and will suggest a follow-up treatment. (Besides, 80% of hernias cure spontaneously.)
The first changes in the intervertebral disc due to overburden are little cracks in the layers around the nucleus. When these cracks heal scar tissue will be developed. Scar tissue however is not as strong as the original tissue. Repeated overburden will finally result in degeneration of the intervertebral disc. The shock absorption will decrease; the intervertebral disc will become thinner because loss of moisture from the nucleus. The cracks in the layers can become so big that the nucleus will lie against the roots of the nerve. This pressure on the roots will cause a radiating pain on the run of the nerve together with numbness and muscle weakness.
We speak of a hernia nucleus pulposus which is the Latin name for bulging intervertebral disc.
On the pictures left and right you see some evident examples of hernias. In practice we do not encounter too often such evident examples. However, even a slight pressure on the intervertebral disc can lead to severe pain. At the moment that failure symptoms occur it is necessary to contact the doctor as soon as possible. Paralysis of leg muscles (not be able to walk on heels or toes) or failure of bladder function and of the sphincter are the most common symptoms. The protrusion of the hernia is so great that the nerves are completely squeezed.
Read more news about a hernia at the site of neurosurgery-zwolle.nl
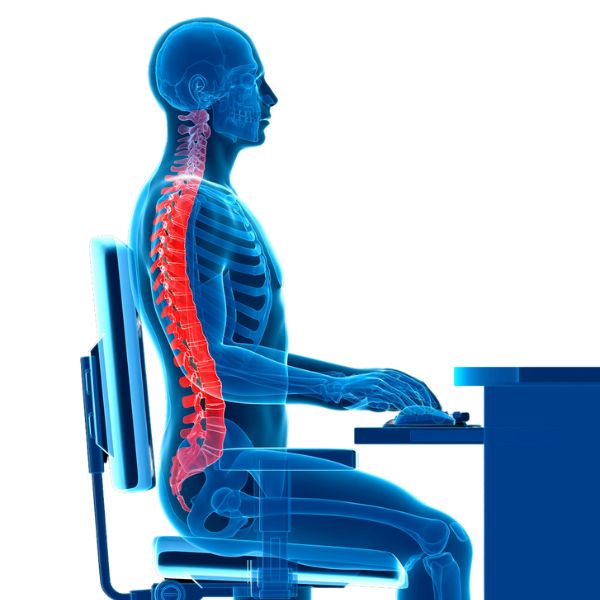
Posture while working
From above story we learn that constantly sitting is too much burden for people suffering from back pain. That’s why a well equipped working place is essential for the treatment of low back pain. On the site VDU you’ll find more information.
General considerations when bending and lifting:
- Lift quietly
- Lift heavy things as close to the body as possible
- Do not lift above shoulder height
- Avoid bending forward too much
- Avoid turning and bending sideways
- Lift with both hands
Picking up objects
Only pick up objects when you can hold on to something fixed to support you. Bend through your knees with a straight back.
Obesity, an important factor
It is a fact that 10 kg overweight will increase the pressure on the intervertebral discs by 40 kg. Physiotherapists use scales which measure beside weights also the fat percentage. Another way is to calculate the Body Mass Index which is based on the relationship between heights and weight. For the treatment of low back pain it is more important to measure the fat percentage than to determine the body mass index.
Physiotherapy and low back pain (directive KNGF)
he physiotherapist differentiates between specific and non-specific low back pain. In case of non-specific low back pain there is no specific physical cause for the pain such as a squeezed nerve or an inflammation.
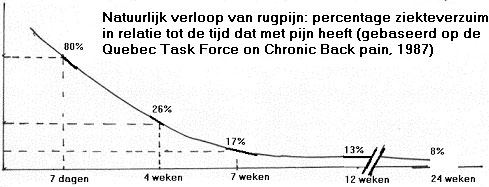
But in 90% of all cases there is no specific cause for the pain. 60% of all people spontaneously suffer from back pain because of a wrong movement (bending or lifting). In 40% the pain gradually increases without apparent cause. Besides stiffness of the back, especially the so called morning stiffness, pain is the main complaint.The natural course of the symptoms is favourable. In 80-90% of the cases the symptoms disappear within 4-6 weeks. For this group physiotherapy is limited to provide information and to give advice for adapted activity.
A different case arises if the complaints after 3 weeks have not diminished but even increased. People then need more rest during the day, take more medicine and are less active. At this stage of the course the physiotherapist will ask when the symptoms started and what you are able to do or not. Sometimes they use questionnaires such as the Quebec Back Pain Disability Scale. The Patient Specific Complaints List (Beurskens) is also used as instrument for determining the severity of your symptoms.
Physiotherapists made a classification of low back pain based on the duration of the pain: acute (0-6 weeks), subacute (7-12 weeks) and chronic (more than 12 weeks). Compared to the classification in stages we see that stage 1 corresponds to the acute period and stage 2 and 3 with the subacute period. The chronic period covers the other stages as described in the beginning of this brochure.
Therapies
According to scientific literature bed rest is not useful as far as acute back pain is concerned. If bed rest really is necessary it’s advised to keep it short (up to two days). The best remedy for acute and subacute low back pain is staying active. In case of chronic back pain exercises will be effective. Exercises in water point out to be effective for patients with chronis back pain.